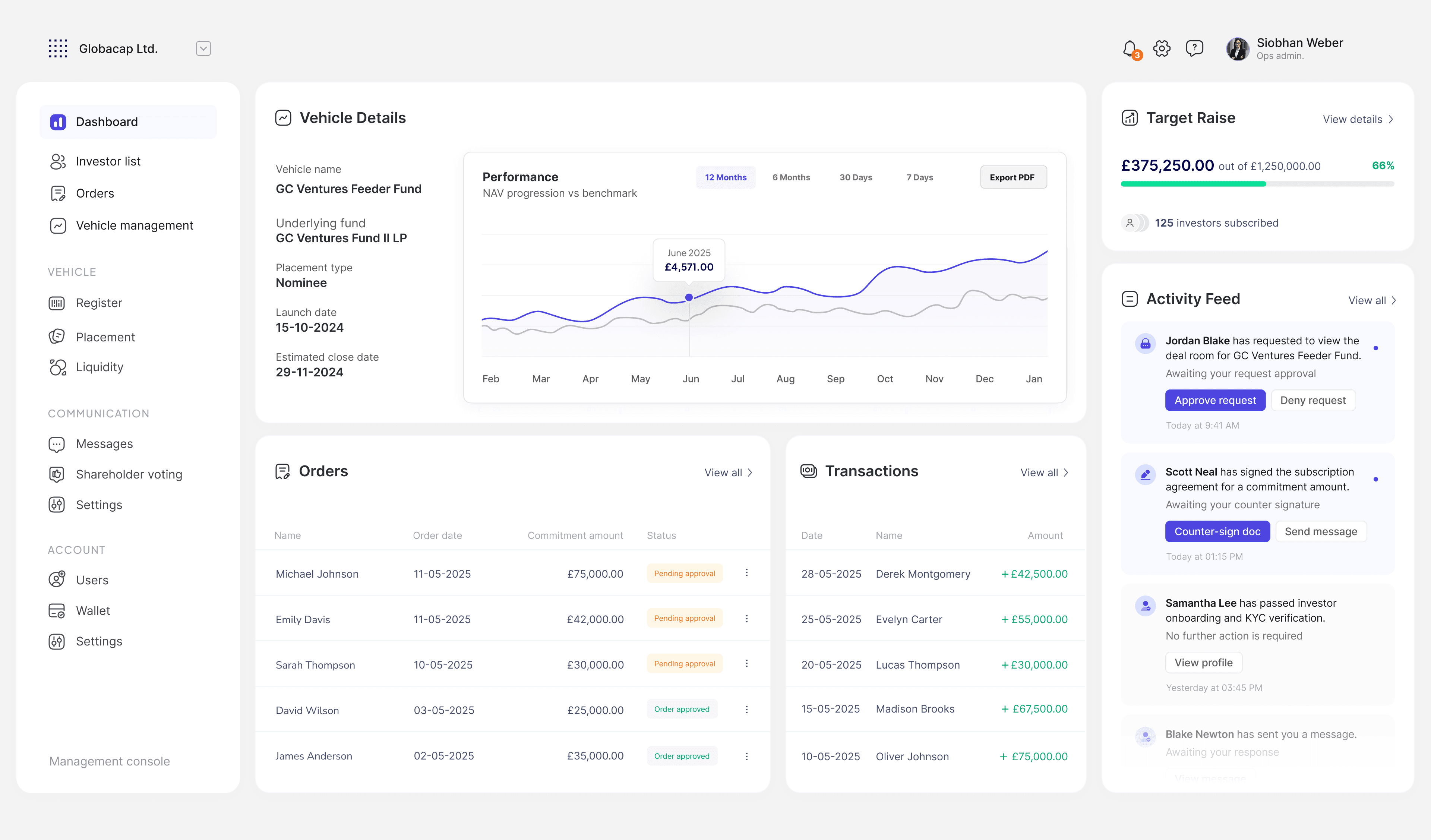
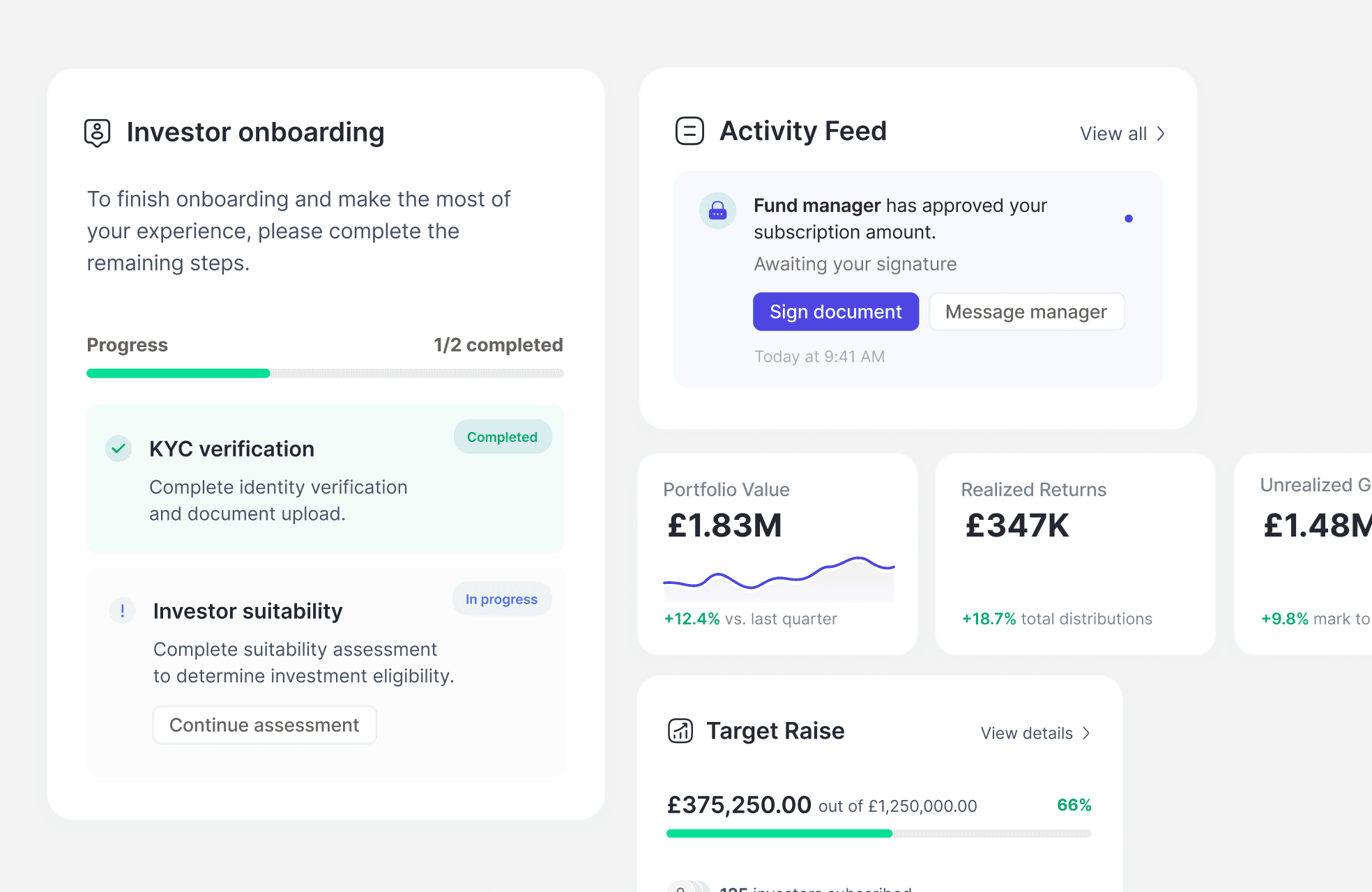
How might we...
replicate the doctor-patient relationship, digitally?
How I added elements of clinical humanity to "treatment request" to be less 'e-commerce' - and reducing abandonment by 43% in the process.
Want to see screens? Skip to the final designs
TLDR
ZavaMed is an online doctor providing accessible healthcare across 7 European markets
Vulnerable patients dealing with weight stigma asked to submit exposing photos. Fraud concerns: photo sharing on Reddit/forums, doctors manually verifying each submission (5-10 min). New GPHC regulations required compliance-we built first-of-its-kind live capture tool instead
THE PROBLEM
22% abandonment, fraud concerns, GPHC regulations, non-supportive UX
THE JOURNEY
BMI photo verification after medical questionnaire and treatment requested.
THE APPROACH
First in-industry Live Capture tool that solves for fraud, safety and vulnerability.
MY ROLE
Product design lead: partnering with PM to prioritise roadmap. Led on research, delivery and execution. Worked closely with: PM, doctors, data team, patient care team, content, commercial.
MY IMPACT
>90%+ photo accuracy (up from ~60%), 160 days/year admin time saved, fraud attempts eliminated, regulations exceeded.
GETTING STARTED
Weight loss stigma and why it's relevant
Society loves to hate on weight loss solutions - almost as much as it loves to hate on weight.
Meal replacement shakes? Tacky. Diet pills? Dangerous. Those vibrating ab belts from infomercials? I actually bought one once. GLP-1s are just the latest thing we’ve dismissed as another ‘get thin quick’ gimmick for people who apparently just “need to try harder”.
Here's what that narrative misses: obesity is a complex chronic disease. Genetics, biology, environment. Not a lack of willpower. I was fully immersed in this space back when I was working with Novo Nordisk on Saxenda and their "Truth About Weight" campaign, which was designed specifically to dismantle weight stigma. The insights from patients were heartbreaking. Because patients don't just face societal prejudice, they face it from doctors too. Dismissed concerns. Assumptions about not trying hard enough. And the added stigma of taking ‘the easy way out’.
Patients don’t take on weight loss treatment lightly.
Not when they’re navigating stigma about their weight, judgement for using medication (taking the easy way out), a healthcare system that treats obesity as a personality defect.
Double the stigma, half the support
But here we are, as ZAVA, trying to offer discreet access to stigmatised treatment. But the barrier required the most exposing act imaginable. I'd been pushing to prioritise BMI verification redesign for months. From my work in this space, I knew exactly what we were asking: strip down, photograph your body, submit it to strangers to prove you deserve treatment for a condition you’re already judged for.
Then the GPHC deadline hit, giving me the leverage I needed to tackle the patient experience problems I'd been flagging all along.
STATS
Patient abandonment
22% cancelled due to discomfort. 17% didn't have scales. 16% lived alone with no one to help. 11% weren't aware it was required.
That’s not confusion, that’s discomfort, lack of trust, and lack of transparency.
STATS
Attempted fraud
Patients submitting old photos, same photo seen across multiple requests, potentially AI images.
Doctors reverse image searching every submission. 5-10 minutes per patient just to verify "yes, this is actually you, recently, not borrowed from Karen in the Facebook group."
STATS
GPHC pressure
22% cancelled due to discomfort. 17% didn't have scales. 16% lived alone with no one to help. 11% weren't aware it was required.
That’s not confusion, that’s discomfort, lack of trust, and lack of transparency.
So the actual brief…
Solve attempted fraud, meet regulations, differentiate from competitors, reduce doctor verification time, work within technical limitations, accommodate 17% without scales, AND preserve patient dignity. Oh and do it fast.
APPROACH
Solving for regulations and fraud prevention: The Live Capture approach
We explored an AI tool claiming 99% BMI accuracy. Sounds good, except it's easily gamed by people actively trying to beat the system (padding jumpers, strategic angles). The tool was designed for fitness enthusiasts who want accurate data. We rejected it. Sometimes the boring human solution is the only one that works.
The technical solution had to stop fraud attempts first: live camera tool. Patients take all photos in real-time. Can't upload old photos, use someone else's image, or submit AI-doctored masterpieces. Date verification automatic. GPHC requirements sorted.
This then left a gaping hole - what about the 17% that didn’t have scales? Before, they had the option of going to a pharmacy to use scales there, then return home to upload their photos. Now they have to upload all three photos at once. Either they buy some scales quick, or get friendly enough with their local Boots that the cashier takes their full body photo for them.
Sometimes you don’t start with the perfect solution - the interim was a supportive dropdown that took them back to the old upload experience. Not ideal, given the other issues with it, but not stopping almost a 5th of our patients.
The full solution is being implemented 6 months later - a ‘save and submit’ feature that allows patients to take images seperately and return to the experience. Patience is a virtue and all that.
Solving for a vulnerable experience
Four principles guided the experience:
Assume nothing.
Don't assume people know what "full-body photo" means, have a mirror, are comfortable alone, or trust us (why would they?). Guide every step
Trust is earned through transparency.
Don't say "don't worry!" when someone is rightfully worried. Say exactly what happens, who sees photos, why they're needed.
Dignity over efficiency.
Let them review, retake, choose who helps. Give them control when they need it most.
Design with the emotion, not against it
This is uncomfortable. Full stop. Design for vulnerability, not fake cheerfulness.
KEY FEATURES
A fully guided journey
Step by step, rather than a huge task reassurance every step of the way start and confirmation page.
KEY FEATURES
Human-first advice
Clear instructions IN CONTEXT Small, bite sized pieces of text A reference image in the top Extra help if needed
KEY FEATURES
Illustrations that detach from body stigma
Using research done by Zalando on their AR try-on feature, they found that using reference illustrations that felt more departed from a ‘true’ human form helped users to detach from any shame they attached to their body type - we debated - should the illustrations show what an eligible BMI should look like? Would that be insulting?
So we went with illustrations that were only vaguely human-like and more geometric, allowing us to illustrate clearly while not forcing further feeligns of shame
KEY FEATURES
Working with rather than against patient context
Patients often said they didn’t have a full length mirror, or a friend/family member to help them take a full-length body picture. So we created two flows - one for patients taking the image themselves, clearly indicating how to set up the phone, and one to guide the person helping.
KEY FEATURES
Trust, trust, trust
Patients were often worried what would happen to their images - nobody wants to upload a medical photo of themselves and not know where its ending up. Data security was also a huge concern. So we over-indexed on trust markers, reassuring languge, and gave patients easy ways to access more information when needed.
TRADE-OFFS
An argument for transparency that I lost
The data was pretty clear: 11.48% cancelled because they didn't know photos would be required. Nearly 12% getting to the end and going "wait, WHAT?"
My argument: be transparent upfront.
Product and Commercial were not fans. It would tank conversion. Our competitors don't mention it either. Why handicap ourselves?
Here's the problem: patients who don't want to upload photos won't finish anyway. Hiding it gives you inflated "placed order" numbers whilst "completed order" numbers stay in the toilet. Plus wasted clinical resource chasing patients and cancelling requests. Transparency captures only patients with true intent. Better metrics where they matter.
I designed an interstitial after treatment request reframing verification as "How we prescribe responsibly." It would manage expectations, explain why, get consent, filter bad actors, position us as careful prescribers.
We built it. Tested it. Ready to ship. Then a senior stakeholder swooped in, declared it "disastrous" for conversion, and killed it. Six months later, we reviewed why patients weren't completing verification. Number one reason by a mile: "I wasn't aware this was required." The killed interstitial would have solved this exact problem.
Turns out pushing people into orders they can’t complete isn't brilliant for conversion. Shocking. I'd love to say being proven right felt satisfying. Mostly it felt like six months of unnecessary frustration that could've been avoided.
Core outcomes
PATIENT ABANDONMENT
>90% photo accuracy (up from 60%), patient feedback shift, significant increase in ‘done’ orders.
Instructions are clearer, patients feel supported, and patients feel confident to continue
ATTEMPTED FRAUD
Fraud attempts eliminated, 5-10 mins doctor time per patient saved, 160+ days of admin time saved
We made this experience better for both patients, doctors, and the patient care team.
GPHC PRESSURE
Guidelines met and exceeded, first among competitors to implement.
I say this with modesty - the experience we drove was best-in-class. Most competitors were relying on much older methods, and we embraced the challenge to go even further.
STILL TO SOLVE FOR
Guidelines met and exceeded, first among competitors to implement.
Better immediate feedback
A place to view images
Transparency upfront
Better entry points
STILL TO SOLVE FOR
Guidelines met and exceeded, first among competitors to implement.
Emerging technology makes fraud still possible, and we need to rise to it
Easier way for doctors to compare and view photos
KEY LEARNINGS
The after-school special moment
This wasn't about making BMI verification "delightful." It's still uncomfortable. Most people would rather not photograph themselves half-dressed and send it to strangers.
But we made it much, much better. We removed barriers, preserved dignity, solved fraud attempts, and met regulations -- multiple difficult things at once without making it any worse.
I fought for transparency and lost. The interstitial got killed. But I still had to ship something that worked, so I focused on what I could control: the experience, the principles, the craft, the support at every step.
Six months later, data proved I was right. But by then, we'd helped thousands of patients navigate one of healthcare's most vulnerable moments. Being proven right doesn't mean you were wrong to compromise. Sometimes you design within constraints, even seeing a better way. You advocate with data, you try to shift the decision. When that doesn't work, you do the absolute best you can with what you've got.
Success isn't winning every argument. It's whether patients felt cared for when they needed it most, and I’m ok pushing back for that.